Contact us today for a consultation with one of our physicians.
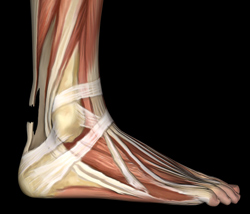
The Achilles tendon or calcaneal tendon is a strong band of fibrous tissue that connects the muscles in the back of your calf to your heel bone. It is the largest tendon in the human body. When the muscle contracts the Achilles tendon tightens allowing you to stand on tiptoe, to point your foot, walk, run, and jump.
When the Achilles tendon tears, the back of your lower leg is affected. It can be ruptured by a sudden force on the foot or ankle. This is most common in people who play sports. The tear may be either partial or complete. In a partial tear, the tendon is still joined to the calf muscle. With a complete tear, connection between the calf muscles and the ankle bone is lost. If you overstretch your Achilles tendon, it can tear completely or partially. If this happens, you might feel a pop or snap, followed by immediate pain in the back of your ankle and lower leg, which will affect your ability to walk properly. If you suspect an Achilles tendon rupture, it is best to see a doctor urgently because the tendon heals better if treated sooner rather than later.
Symptoms may come suddenly during an activity or injury and it's also possible to have no signs or symptoms with an Achilles tendon rupture. The pain settles quickly, but you are left with an aching pain in the lower leg. After the injury, the usual symptoms are as follows:
The injury can happen in different ways, for example; making a forceful push (starting a race or jumping), a sudden trip causing overstretch of the tendon, falling from a significant height, stepping into a hole or stepping off a curb.
Sometimes the Achilles tendon is weak, making it more prone to rupture. There are factors that can increase your risk of Achilles tendon rupture, these include:
There are two options for treatment, non-surgical and surgical but eventually surgery is the best option to repair an Achilles tendon rupture. Surgically the doctor repairs the tendon sewing together the torn ends of the Achilles tendon, and sometimes may use another tendon or a tendon graft to help with the repair. A plaster cast or brace (orthosis) is needed after the operation. The non-surgical approach involves casting, special braces, orthotics, and physical therapy, allowing the tendon to heal naturally in a brace or cast, but if the tendon doesn’t heal on its own, a surgical repair is done at a later time. Non-surgical treatment is often used for non-athletes, for those with a low level of physical activity, the elderly and those with complicating medical conditions. It is important to diagnose and treat this injury as soon as possible, to help promote healing. Treatment involves wearing a plaster cast or brace (orthosis) for about six to eight weeks. Both options involve having a cast or a brace for weeks, to protect the tendon while it heals.
In general, the prognosis is good. The tendon does need time to heal, usually about six to eight weeks, and more time would be needed to allow the muscles to regain normal strength after being in a plaster cast or a brace. There are possible complications in whichever treatment option is used. With the non-surgical approach there is a chance that the Achilles tendon will not heal fully and further treatment such as surgery may be needed. For the surgical approach, as in any surgical treatment these are usually minor complications such as a wound infection or reduced sensation near the operation site. There is a chance that the tendon may scar or may become shorter during the healing process, or it could become torn again later.
For more information about the foot conditions we can treat in the Los Angeles and Beverly Hills, CA area, including bunions, hammertoe and Morton's neuroma, please contact us at 855-SOMA-844 (855-766-2844).